Society
Doctors managed to change blood type in an organ for the first time: details
Canadian transplant surgeons have found a way to safely change the second type of blood in donor organs to the first. This could reduce the percentage of patients who wait long periods for surgery.
The first case was described by doctors from the Toronto Hospital Research Institute in a report published in the journal Science. So, during the transformation, human lungs came to the laboratory from a patient with the second blood type, but left the laboratory already with the first type.
Scientists believe they have come close to creating "universal" organs that would fit any patient.
Currently, people who need a transplant are placed on a waiting list. Finding donor organs for transplantation is a very difficult task. And it is not just because there are not enough donors for all patients. Not all organs are suitable for every specific person because of antigen incompatibility.
It is known that the blood group is determined by the presence of antigens on the surface of red blood cells. Type A blood (type II) contains antigen A, B blood (type III) has antigen B, AB blood (type IV) has both antigens, while 0 blood (type I) has none.
Description:
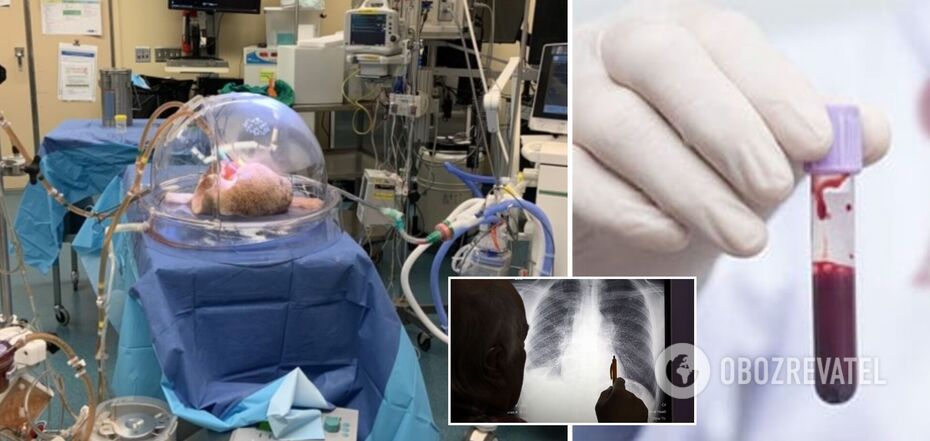
Scientists have been able to change the second blood type in an organ to a first blood type.
Source:
Rihabay
Alt:
The most common blood type in the world is type O-negative (0+), with 39% of the world's population (approximately 3 billion people). AB- is the least common blood type, with only about 32 million people (0.4% of the population) having this type of blood. Rh-negative is found in less than 7% of people, but in the U.S. the proportion of people with Rh- reaches 16%, and in New Zealand it is 18%.
In the experiment, using donor lungs, medics injected a small dose of certain enzymes into the tissue. The team then performed antibody staining, which flagged the remaining antigens so they could see how successful they were. Within an hour, more than 90 percent of the second blood group antigens had been destroyed. Four hours later, that number had risen to 97.
"This technically changes the blood type of these lungs to first," the scientists explained.
For now, however, the technology only works for blood type two; plans are underway to create the same technology for blood type three.
"The technology made it possible to 'nullify' these antigens in the donor lung tissue and obtain a universal first blood group," the researchers added.
Transfusions are known to require blood of the same group as the recipient's, or group 0, otherwise severe complications are possible.
Ahead of the researchers have experiments to transplant such organs on mice, and then - on humans. Clinical trials are planned to be completed in a year and a half.
As reported by OBOZREVATEL, scientists told what foods should not be eaten by people with a certain blood group.
Description:
Address by the OBOZREVATEL team
Source: Alt: